Jorge Planas, M.D., Emilia Migliano, M.D., Jorge Wagenfuhr, Jr., M.D., and Sebastian Castillo, M.D.
Barcelona, Spain. Breast implant capsular contractures 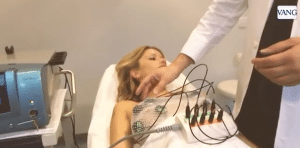
Abstract. The authors report their experience on the non surgical treatment of capsular contractures due to breast implant augmentation mammaplasty. External ultrasonic repeated applications have been applied to 24 patients after closed capsulotomy procedures in order to reduce the recurrency rates. The new ultrasonic device used was based on a 2-MHz generator with a timing adjustable power emission connected to eight transducers designed for breast anatomy. The authors report significant improvement of the closed capsulotomy technique demonstrating a persistent stability of the achieved results in 82% of the treated contractures, even in severe cases (Baker’s IV), after a minimum follow-up period of 12 months. Methods of application, technical features of the ultrasonic device, experimental charts, and results obtained on 34 Breast implant capsular contractures are reported and discussed.
Key words: Ultrasonic treatment-Breast implant-Capsular contracture-Closed capsulotomy
Introduction
Breast implant capsular contracturess is a wellknown complication of augmentation mamoplasty. The etiologic aspects of this multifactorial process are still unclear: the contracture can occur uni- or bilaterally, within weeks to years after surgery developing to various degrees of severity often asymmetrically [3,8,13].
The improvement of implant design, filling materials, and surface coatings has contributed to the reduction of the postsurgical contracture rate [4,5,9]. In the same way, technical variations of the surgical placement of the implants and several drug administration have been recommended for the prevention of fibrous capsule contracture [8,9,13]. Although significant results have been obtained, lowering the percentage of contracture, the risk still exists.
Presented in part at the annual meeting of the Spanish Society of Aesthetic Plastic Surgery. Barcelona, 27-30th April 1997 Correspondence to Dr. Jorge Planas, M.D., Clinica Planas, Pere de Montcada 16, 08034 Barcelona, Spain
When a fibrous capsular contracture becomes clinically evident, the closed capsulotomy is considered one of the most effective, nonsurgical treatment, especially if followed by repeated massages of the breast [1,8,12,13]. As reported by Baker [1,2] the closed compression technique can only fail in a few severe cases, but has a 33% of recurrency rate within 12 months. Posttreatment massages can, in fact, delay but not prevent a new fibrotic process of healing of the ruptured capsule.
In Breast implant capsular contracturess theExternal ultrasonic treatment has been proved to be effective on the biological mechanisms of wound healing and is actually used with significant results in disorders such as cellulitis, keloidal scarring, sclerodermia, Dupuytren’ s, and Peyronie’ s diseases or in posttraumatic and degenerative joint alterations [10,11,14,15].
Two years ago we started to apply the external ultrasonic treatment with a modified device and a new experimental protocol. We tested if ultrasonic irradiation would be effective even in the treatment of the most severe cases of Breast implant capsular contracturess preventing the recurrencies.
Materials and Methods
We have treated 24 patients (age ranging from 24 to 52 years, average 36.8) with a total amount of 34 contractured breast implants (14 unilateral and 10 bilateral) classified in various degrees of contractures according to the Baker’s scale as reported in Table 1. Eighteen patients have the implants positioned prepectorally, three patients
Table 1. Distribution of the contractures before treatment according to the Baker’s scale
Fig. 1. The ultrasonic device with eight transducers used for the treatment.
retropectorally, two patients were postmastectomy reconstructions with implants, and the placement of the prosthesis is unknown in one patient.
From the 34 prosthesis, 23 were silicone gel, four soja oil, and seven unknown. The contractures have developed within 22 weeks to 4 years with an average of 6 months after the surgical augmentation procedure.
All the contractured breasts have undergone a primary closed capsulotomy according to the manual compression technique reported by Baker et al. in 1976 [1]. In three cases, with severe contracture (IV degree), the closed capsulotomy was unsuccessful; however, after a single ultrasonic session, the capsulotomy was effective. We have used an ultrasonic device applied before for multipurpose superficial soft-tissue treatment (cellulitis, keloidal scarring).
We have set this appliance to reach deep layers of fibrotic tissues providing it with a 2-MHz generator. The ultrasonic device was connected to eight transducers for the ultrasonic emission with an adjustable power per outlet varying from 1 to 15 W to produce a maximum power density of 3W/cm2 (Fig. 1). On each breast were applied four transducers oriented toward the capsule and fixed on a special designed bra (Fig. 2).
The ultrasonic device could be set in continuous or pulsed emission way. In any case, once the values of power emission per outlet and of total ultrasonic energy to produce have been set, the appliance ca1culated automatically the duration of the cycle needed to distribute it to the transducers. In pul sed position the emission cycle is up to five times longer, in order to minimize the overheating effect of ultrasonic energy on biological tissues. By administering the same total amount of ultrasonic energy, we have used initially either continuous or pul sed emission. The latter has been preferred for further experimentation because it produced better clinical results in terms of mammary softening and did not cause unpleasant overheating feeling to the patients. The setting ofthe ultrasonic device used were 15 Watts ofpower per outlet at any cycle with a power density at any trans
Capsular Contractures
Fig. 2. A 30-year-old patient with bilateral breast capsular contracture treated with the extemal ultrasonic device.
ducer of 600 mW/cm2. We have varied the number of cycles of ultrasonic applications per session in respect of the severity of the contracture and the number of ultrasonic sessions considering the clinical response. The ultrasonic treatment session has been scheduled two times a week until a good and stable result has been obtained. This required sessions of average 5.27 with 15-36 cycles of ultrasonic application for each session.
Results
The results obtained applying this technique, with repeated applications of ultrasonic energies at the average follow-up of 12 months are reported in Tables 2 and 3. We did not have any kind of complication concerning either the capsulotomy or the ultrasonic administration. The patients referred, after the ultrasonic session, subjective softening of the breast without any unpleasant over-heating feeling. In three cases (Baker’s IV), the closed compression capsulotomy had been effective only after one session of the ultrasonic treatment.
Discussion
The most comprehensive long-term report regarding the results of closed-compression capsulotomy has been published by Little and Baker in 1980 [12]. They have reported on a wide sample of patients where the higher recurrency rate of posttreatment capsular contracture can be detected within 6 months and where the overall recurrencies at 12 months can be stated at least at 33%. Only the 67% of the treated patients, regardless of the pretreatment severity of the contracture have obtained a good and long-lasting result. In our series, even if with a smaller sample of patients, we have obtained an overall 82.27% of patients free of clinical signs of capsular contracture at the 12 months follow-up (see Table 3). Moreover, these dates have to be confirmed considering the severity of the treated contractures. In the Baker’ s report, we can ca1culate that the more severe cases (III and IV)
Table 2. Pre- and posttreatment distribution of the contractures according to the Baker’ s scale, with the percentage of improvement for each degree
degree) were about 62%, and this percentage is rea11y lower with respect to that of our series (97%, see Table 1).
The analysis after 1 year offo11ow-up (see Table 2 and 3) demonstrate obviously that patients with severe contracture have les s stability of the results but even in IV degree sample, the percentage of asymptomatic patients is over 72%. The administration of external ultrasonic energy has been proved to be effective in the modulation of fibrous tissue healing processes. Ultrasound, in spite of microwaves can reach deep layers of tissues with higher energy easier. They usua11y produce three kind of effects on the biological tissues: mechanical, thermical, and biochemical. The last two are secondary to the first but at the used levels of energy, they are the most useful for the modulation of biological processes. The thermical effect increases the speed of ce11ular metabolism and has been proven to stimulate the fibroblast activation and the wound healing [10,14]. In continuous emission, the thermical effect can be so high as to produce protein denaturation and burns. We have preferred the pul sed emission to avoid this kind of complication and because this type of administration produces the best results in terms of biological and physiologic processes modulation [7,10]. These beneficial effects have been related to tissular blood flow and oxygenation increase, release of inflammation ce11ular mediators, increase of fibrolytic processes with a higher turnover of co11agen proteins [6,10,15]. It is we11 known that the effects of the external ultrasonic administrations are maximized at the interface
between two layers of tissues with different characteristics of acoustic impedance. The contracted fibrous capsule and the mammary implant surface are a we11-defined acoustic interface. Moreover, a recent report by Lelesne [11] has demonstrated that there is a high rate of silicone
droplets enclosed in the capsular tissues. In our opinion, a11 these events can significantly contribute to change the implant capsular structure improving tissular metabolism and preventing its fibrotic contracture.
Conclusions
The results obtained with this work can confirm the clinical evidence of capsular softening and an easier closed capsulotomy, which can be achieved after the external ultrasonic treatment. We believe that this kind of application can be useful either for the treatment of mammary
Table 3. Percentage of improvement after treatment with 1 year follow-up
implant fibrotic contractures or for the prevention of postcapsulotomy recurrencies. Furthermore, the external ultrasonic treatment has proved to be easy to apply, we11 accepted by the patient, cost-effective, and free of significant complications.
Acknowledgment. We are grateful to Prof. J.R. Zaragoza and Dr. F. Govoni for their help and cooperation. The ultrasonic device, named Capsulotomus, has been developed by Mediform, Spain.
References
- Baker JL, Bartels RJ, Douglas WM: Closed compression technique for rupturing a contracted capsule around a breast implant. Plast Recontr Surg 58: 137, 1976
- Baker JL, Chandler ML, Le Vier RR: Occurrence and activity of myofibroblasts in human capsular tissue surrounding mammary implants. Plast Recontr Surg 68:905, 1981
- Burkhardt BR: Capsular contracture: hard breasts, soft data. Clin Plast Surg 15:521, 1988
- Burkhardt BR, Eades E: The effect of Biocell texturing and povidone-iodine irrigation on capsular contracture around saline-inflatable breast implants. Plast Recontr Surg 96:1317,1995
- Caffee HH, Rotatori DS: Intracapsular injection of triamcinolone for prevention of the contracture. Plast .Recontr Surg 92: 1073, 1993
- Carpaneda CA: Inflammatory reaction and capsular contracture around smooth silicone implants. Aesth Plast Surg 21:110,1997
- Chatter BV, Williams AR: Platelet aggregation induced invitro by therapeutic ultrasound. Tromb Haemost 38:640, 1977
- Georgiade NG: Aesthetic surgery of the breast. Philadelphia: WB Saunders Co., 1990
- Handel N, Jensen A, Black Q: The fate of breast implants: a critical analysis of complications and outcomes. Plast Recontr Surg 96:1521, 1995
- Lehmann JF, De Lauter BJ: Diatermia y terapeutic superficial con calor, laser y frio. In Krusen J, 4 ed. Medicina fisica y rehabilitation. Madrid: Editorial Medica Panamericana, 1994
- Lelesne CB: Textured surface silicone breast implants: histology in the humano Aesth Plast Surg 21:93, 1997
- Little G, Baker JL: Results of closed compression capsulotomy for treatment of contracted breast implant capsules. Plast Recontr Surg 65:30, 1980
- McCarthy JG: Plastic Surgery, Vol. VI. Philadelphia: WB Saunders Co., 1990
- Scott WW, Scardino PL: A new concept in the treatment of Peyronie’s disease. South Med J 41:173, 1948
- Williams AR, Chater BV, Allen KA, Sanderson JH: The use of 13 tromboglobulin to detect platelet damage by therapeutic ultrasound in vivo. J Clin Ultrasound 9:145, 1981

